Featured Post
Who Can Own a Medical Spa?

Show your committment to patient safety, legal compliance and community over competition.
AmSpa members receive preferred pricing on all AmSpa live and virtual trainings.
Get the latest news and information about safe, legal practice in medical aesthetics directly in your inbox.
Get access to med spa laws, in-person and online training and more!

Marketing
By Aesthera MarketingThe way people choose a med spa today looks nothing like it did a few years ago. Many ...

AmSpa Events
By Adam Reinebach, Chief Executive Officer, American Med Spa Association As we close the first quarter of 2026, more people are ...

AmSpa Events
Choosing the right classes at Medical Spa Show 2026 can fast-track your next phase of growth. Whether you just opened ...

Marketing
By Salt MarketingJust a few months ago, JAG Medical Spa in Summerville, South Carolina was doing everything “right” on Instagram ...


Marketing
By AestheticsPro For medical spa owners looking to reach their clients in the most...
Top Tags
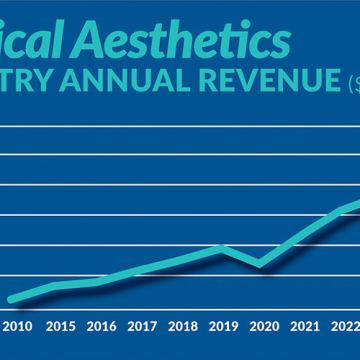
January 24, 2023
Figure displays medical aesthetics industry annual revenue ($ in billions). By Madilyn Moeller Day-to-day life...
February 24, 2021
By Bradford E. Adatto, Partner, ByrdAdattoIntravenous (IV) therapy has been used to provide nutrition and...

September 21, 2023
By Patrick O'Brien, JD, General Counsel, American Med Spa Association [AmSpa first published a...
July 19, 2023
By Patrick O'Brien, General Counsel, American Med Spa Association (AmSpa) UPDATE #2 (2/08/2024): Since...